- Diabetes, obesity and metabolism
- Performance of Simple Fibrosis Score in Non-Alcoholic Fatty Liver Disease with and without Type 2 Diabetes
-
Seung Min Chung, Min Kyu Kang, Jun Sung Moon, Jung Gil Park
-
Endocrinol Metab. 2023;38(2):277-281. Published online March 13, 2023
-
DOI: https://doi.org/10.3803/EnM.2022.1635
-
-
1,873
View
-
98
Download
-
1
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- This cross-sectional study enrolled 267 patients with metabolic risk factors and established non-alcoholic fatty liver disease in the prospective cohort. The performance of fibrosis-4 (FIB-4) score (≥1.3) to diagnose advanced fibrosis using transient elastography (liver stiffness measurement [LSM] ≥8 kPa) was analyzed. Comparing patients with type 2 diabetes (T2D, n=87) and without (n=180), not FIB-4, but LSM was significantly higher in T2D (P=0.026). The prevalence of advanced fibrosis was 17.2% in T2D and 12.8% in non-T2D. FIB-4 exhibited higher proportion of false negatives in T2D patients (10.9%) than those without (5.2%). The diagnostic performance of FIB-4 was suboptimal in T2D (area under curve [AUC], 0.653; 95% confidence interval [CI], 0.462 to 0.844) compared to that in non-T2D (AUC, 0.826; 95% CI, 0.724 to 0.927). In conclusion, patients with T2D might be beneficial to conduct transient elastography without screening to avoid missing advanced fibrosis.
-
Citations
Citations to this article as recorded by  - Multiple Definitions of Fatty Liver Disease: Which One Most Accurately Predicts Diabetes?
Eun-Jung Rhee
Endocrinology and Metabolism.2024; 39(2): 397. CrossRef - Prevalence of High and Moderate Risk of Liver Fibrosis Among Patients With Diabetes at a Noncommunicable Diseases (NCD) Clinic in a Primary Healthcare Center in Northern India
Anubhav Mondal, Aninda Debnath, Ghurumourthy Dhandapani, Abhishek Sharma, Shveta Lukhmana, Geeta Yadav
Cureus.2023;[Epub] CrossRef
- Miscellaneous
- Immune Checkpoint Inhibitors and Endocrine Disorders: A Position Statement from the Korean Endocrine Society
-
Hyemi Kwon, Eun Roh, Chang Ho Ahn, Hee Kyung Kim, Cheol Ryong Ku, Kyong Yeun Jung, Ju Hee Lee, Eun Heui Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Jun Sung Moon, Jin Hwa Kim, Mi-kyung Kim, The Committee of Clinical Practice Guideline of the Korean Endocrine Society
-
Endocrinol Metab. 2022;37(6):839-850. Published online December 26, 2022
-
DOI: https://doi.org/10.3803/EnM.2022.1627
-
-
3,581
View
-
322
Download
-
2
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
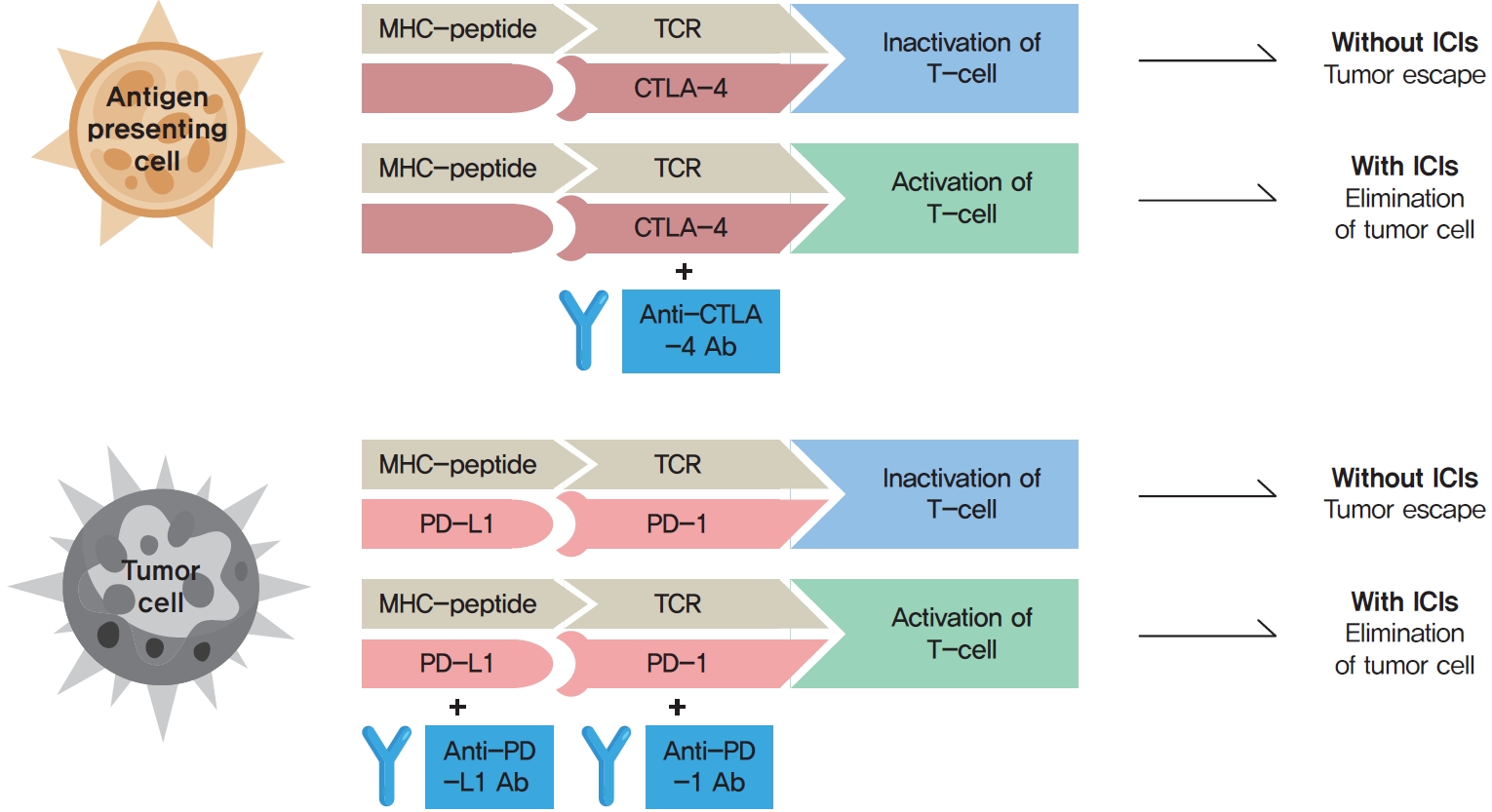
- Immune checkpoint inhibitors (ICIs) including an anti-cytotoxic T-lymphocyte-associated antigen 4 inhibitor, anti-programmed cell death protein 1 (PD-1) inhibitors, and anti-PD-ligand 1 inhibitors are representative therapeutics for various malignancies. In oncology, the application of ICIs is currently expanding to a wider range of malignancies due to their remarkable clinical outcomes. ICIs target immune checkpoints which suppress the activity of T-cells that are specific for tumor antigens, thereby allowing tumor cells to escape the immune response. However, immune checkpoints also play a crucial role in preventing autoimmune reactions. Therefore, ICIs targeting immune checkpoints can trigger various immune-related adverse events (irAEs), especially in endocrine organs. Considering the endocrine organs that are frequently involved, irAEs associated endocrinopathies are frequently life-threatening and have unfavorable clinical implications for patients. However, there are very limited data from large clinical trials that would inform the development of clinical guidelines for patients with irAEs associated endocrinopathies. Considering the current clinical situation, in which the scope and scale of the application of ICIs are increasing, position statements from clinical specialists play an essential role in providing the appropriate recommendations based on both medical evidence and clinical experience. As endocrinologists, we would like to present precautions and recommendations for the management of immune-related endocrine disorders, especially those involving the adrenal, thyroid, and pituitary glands caused by ICIs.
-
Citations
Citations to this article as recorded by  - Pembrolizumab plus lenvatinib for radically unresectable or metastatic renal cell carcinoma in the Japanese population
Ryo Fujiwara, Takeshi yuasa, kenichi kobayashi, tetsuya yoshida, susumu kageyama
Expert Review of Anticancer Therapy.2023; 23(5): 461. CrossRef - Incidence of Endocrine-Related Dysfunction in Patients Treated with New Immune Checkpoint Inhibitors: A Meta-Analysis and Comprehensive Review
Won Sang Yoo, Eu Jeong Ku, Eun Kyung Lee, Hwa Young Ahn
Endocrinology and Metabolism.2023; 38(6): 750. CrossRef
- Miscellaneous
- COVID-19 Vaccination for Endocrine Patients: A Position Statement from the Korean Endocrine Society
-
Cheol Ryong Ku, Kyong Yeun Jung, Chang Ho Ahn, Jun Sung Moon, Ju Hee Lee, Eun Heui Kim, Hyemi Kwon, Hee Kyung Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Eun Roh, Jin Hwa Kim, Mi-kyung Kim, the Committee of Clinical Practice Guideline of the Korean Endocrine Society
-
Endocrinol Metab. 2021;36(4):757-765. Published online August 17, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.404
-
-
10,447
View
-
419
Download
-
19
Web of Science
-
21
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Since the first outbreak of coronavirus disease 2019 (COVID-19), ongoing efforts have been made to discover an efficacious vaccine against COVID-19 to combat the pandemic. In most countries, both mRNA and DNA vaccines have been administered, and their side effects have also been reported. The clinical course of COVID-19 and the effects of vaccination against COVID-19 are both influenced by patients’ health status and involve a systemic physiological response. In view of the systemic function of endocrine hormones, endocrine disorders themselves and the therapeutics used to treat them can influence the outcomes of vaccination for COVID-19. However, there are very limited data to support the development of clinical guidelines for patients with specific medical backgrounds based on large clinical trials. In the current severe circumstances of the COVID-19 pandemic, position statements made by clinical specialists are essential to provide appropriate recommendations based on both medical evidence and clinical experiences. As endocrinologists, we would like to present the medical background of COVID-19 vaccination, as well as precautions to prevent the side effects of COVID-19 vaccination in patients with specific endocrine disorders, including adrenal insufficiency, diabetes mellitus, osteoporosis, autoimmune thyroid disease, hypogonadism, and pituitary disorders.
-
Citations
Citations to this article as recorded by  - COVID-19 mRNA vaccine may trigger subacute thyroiditis
Mehmet Sözen, Ömercan Topaloğlu, Berrin Çetinarslan, Alev Selek, Zeynep Cantürk, Emre Gezer, Damla Köksalan, Taner Bayraktaroğlu
Human Vaccines & Immunotherapeutics.2024; 17(12): 5120. CrossRef - The role of co-morbidities in the development of an AEFI after COVID-19 vaccination in a large prospective cohort with patient-reported outcomes in the Netherlands
C. Ouaddouh, J.W. Duijster, T. Lieber, F.P.A.M. van Hunsel
Expert Opinion on Drug Safety.2024; 23(3): 323. CrossRef - Thyroid dysfunction in COVID-19
David Tak Wai Lui, Chi Ho Lee, Yu Cho Woo, Ivan Fan Ngai Hung, Karen Siu Ling Lam
Nature Reviews Endocrinology.2024;[Epub] CrossRef - Adult-Onset Type 1 Diabetes Development Following COVID-19 mRNA Vaccination
Hyeyeon Moon, Sunghwan Suh, Mi Kyoung Park
Journal of Korean Medical Science.2023;[Epub] CrossRef - Prior immunization status of COVID-19 patients and disease severity: A multicenter retrospective cohort study assessing the different types of immunity
Javaria Aslam, Faisal Shahzad Khan, Muhammad Talha Haris, Hewad Hewadmal, Maryam Khalid, Mohammad Y. Alshahrani, Qurrat-ul-ain Aslam, Irrum Aneela, Urooj Zafar
Vaccine.2023; 41(2): 598. CrossRef - Mortality and Severity of Coronavirus Disease 2019 in Patients with Long-Term Glucocorticoid Therapy: A Korean Nationwide Cohort Study
Eu Jeong Ku, Keeho Song, Kyoung Min Kim, Gi Hyeon Seo, Soon Jib Yoo
Endocrinology and Metabolism.2023; 38(2): 253. CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef - Inactivated SARS-CoV-2 vaccination does not disturb the clinical course of Graves’ disease: An observational cohort study
Shichen Xu, Huixin Yu, Xian Cheng, Jing Wu, Jiandong Bao, Li Zhang
Vaccine.2023; 41(38): 5648. CrossRef - Adrenal Crisis Associated With COVID-19 Vaccination in Patients With Adrenal Insufficiency
Yukako Kurematsu, Takako Mohri, Sadanori Okada, Yutaka Takahashi
JCEM Case Reports.2023;[Epub] CrossRef - Adverse Events Associated with COVID-19 Vaccination in Adolescents with Endocrinological Disorders: A Cross-Sectional Study
İbrahim Mert Erbaş, İrem Ceren Erbaş, Gözde Akın Kağızmanlı, Kübra Yüksek Acinikli, Özge Besci, Korcan Demir, Ece Böber, Nurşen Belet, Ayhan Abacı
Journal of Clinical Research in Pediatric Endocrinology.2023; 15(3): 248. CrossRef - Neue Aspekte der Glukokortikoidsubstitution bei Nebennierenrindeninsuffizienz
Tina Kienitz, Gesine Meyer
Der Internist.2022; 63(1): 12. CrossRef - Endocrine Follow-up During Post-Acute COVID-19: Practical Recommendations Based on Available Clinical Evidence
Rimesh Pal, Ameya Joshi, Sanjay K. Bhadada, Mainak Banerjee, Suresh Vaikkakara, Satinath Mukhopadhyay
Endocrine Practice.2022; 28(4): 425. CrossRef - Safety of Inactivated and mRNA COVID-19 Vaccination Among Patients Treated for Hypothyroidism: A Population-Based Cohort Study
Xi Xiong, Carlos King Ho Wong, Ivan Chi Ho Au, Francisco Tsz Tsun Lai, Xue Li, Eric Yuk Fai Wan, Celine Sze Ling Chui, Esther Wai Yin Chan, Franco Wing Tak Cheng, Kristy Tsz Kwan Lau, Chi Ho Lee, Yu Cho Woo, David Tak Wai Lui, Ian Chi Kei Wong
Thyroid.2022; 32(5): 505. CrossRef - The New Entity of Subacute Thyroiditis amid the COVID-19 Pandemic: From Infection to Vaccine
Mihaela Popescu, Adina Ghemigian, Corina Maria Vasile, Andrei Costache, Mara Carsote, Alice Elena Ghenea
Diagnostics.2022; 12(4): 960. CrossRef - Adrenal Crisis Secondary to COVID-19 Vaccination in a Patient With Hypopituitarism
Nikolina Markovic, Anila Faizan, Chirag Boradia, Sridhar Nambi
AACE Clinical Case Reports.2022; 8(4): 171. CrossRef - The Effect of Inactivated SARS-CoV-2 Vaccines on TRAB in Graves’ Disease
LingHong Huang, ZhengRong Jiang, JingXiong Zhou, YuPing Chen, HuiBin Huang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Osteoporosis in Patients With Respiratory Diseases
Yue Ma, Shui Qiu, Renyi Zhou
Frontiers in Physiology.2022;[Epub] CrossRef - Pilot Findings on SARS-CoV-2 Vaccine-Induced Pituitary Diseases: A Mini Review from Diagnosis to Pathophysiology
Ach Taieb, El Euch Mounira
Vaccines.2022; 10(12): 2004. CrossRef - Forty Years Together, New Leap Forward! The 40th Anniversary of the Korean Endocrine Society
Jong Chul Won, Ki-Hyun Baek
Endocrinology and Metabolism.2022; 37(6): 851. CrossRef - No need of glucocorticoid dose adjustment in patients with adrenal insufficiency before COVID-19 vaccine
Tania Pilli, Cristina Dalmiglio, Gilda Dalmazio, Alfonso Sagnella, Raffaella Forleo, Lucia Brilli, Fabio Maino, Cristina Ciuoli, Maria Grazia Castagna
European Journal of Endocrinology.2022; 187(1): K7. CrossRef - Diabetes and COVID-19 Vaccination
Hae Dong Choi, Jun Sung Moon
The Journal of Korean Diabetes.2021; 22(4): 221. CrossRef
- Diabetes, Obesity and Metabolism
- High Fibrosis-4 Index Is Related with Worse Clinical Outcome in Patients with Coronavirus Disease 2019 and Diabetes Mellitus: A Multicenter Observational Study
-
Sung-Woo Kim, Jae-Han Jeon, Jun Sung Moon, Mi Kyung Kim
-
Endocrinol Metab. 2021;36(4):800-809. Published online August 20, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.1040
-
-
5,115
View
-
176
Download
-
6
Web of Science
-
5
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
Based on recent evidence on the importance of the presence of diabetes mellitus (DM) and fibrosis-4 (FIB-4) index in coronavirus disease 2019 (COVID-19) mortality, we analyzed whether these factors could additively predict such mortality.
Methods
This multicenter observational study included 1,019 adult inpatients admitted to university hospitals in Daegu. The demographic and laboratory findings, mortality, prevalence of severe disease, and duration of quarantine were compared between patients with and without DM and/or a high FIB-4 index. The mortality risk and corresponding hazard ratio (HR) were analyzed using the Kaplan-Meier method and Cox proportional hazard models.
Results
The patients with DM (n=217) exhibited significantly higher FIB-4 index and mortality compared to those without DM. Although DM (HR, 2.66; 95% confidence interval [CI], 1.63 to 4.33) and a high FIB-4 index (HR, 4.20; 95% CI, 2.21 to 7.99) were separately identified as risk factors for COVID-19 mortality, the patients with both DM and high FIB-4 index had a significantly higher mortality (HR, 9.54; 95% CI, 4.11 to 22.15). Higher FIB-4 indices were associated with higher mortality regardless of DM. A high FIB-4 index with DM was more significantly associated with a severe clinical course with mortality (odds ratio, 11.24; 95% CI, 5.90 to 21.41) than a low FIB-4 index without DM, followed by a high FIB-4 index alone and DM alone. The duration of quarantine and hospital stay also tended to be longer in those with both DM and high FIB-4 index.
Conclusion
Both DM and high FIB-4 index are independent and additive risk factors for COVID-19 mortality.
-
Citations
Citations to this article as recorded by  - COVID-19 and hepatic injury: Diversity and risk assessment
Fares E M Ali, Mostafa K Abd El-Aziz, Mahmoud M Ali, Osama M Ghogar, Adel G Bakr
World Journal of Gastroenterology.2023; 29(3): 425. CrossRef - Differential Effects of COVID-19 Hospitalization on the Trajectory of Liver Disease Progression
Dilara Hatipoğlu, Connor Mulligan, Jeffrey Wang, Juan Peticco, Reid Grinspoon, Sanjay Gadi, Camilla Mills, Jay Luther, Raymond T. Chung
Gastro Hep Advances.2023; 2(4): 480. CrossRef - Association of non-alcoholic fatty liver and metabolic-associated fatty liver with COVID-19 outcomes: A systematic review and meta-analysis
Gowthami Sai Kogilathota Jagirdhar, Rakhtan K Qasba, Harsha Pattnaik, Kaanthi Rama, Akshat Banga, Shiva Teja Reddy, Anna Carolina Flumignan Bucharles, Rahul Kashyap, Praveen Reddy Elmati, Vikas Bansal, Yatinder Bains, Theodore DaCosta, Salim Surani
World Journal of Gastroenterology.2023; 29(21): 3362. CrossRef - COVID-19 and Fatty Liver Disorders
Maria Guarino, Valentina Cossiga, Francesco Cutolo, Maria Attanasio, Raffaele Lieto, Filomena Morisco
Journal of Clinical Medicine.2023; 12(13): 4316. CrossRef - Prevalence and Prognostic Significance of Liver Fibrosis in Patients With Aneurysmal Subarachnoid Hemorrhage
Tiangui Li, Peng Wang, Xiao Gong, Weelic Chong, Yang Hai, Chao You, Juan Kang, Fang Fang, Yu Zhang
Frontiers in Neurology.2022;[Epub] CrossRef
- Clinical Study
- Fasting Plasma Glucose Level Independently Predicts the Mortality of Patients with Coronavirus Disease 2019 Infection: A Multicenter, Retrospective Cohort Study
-
Min Cheol Chang, Jong-Moon Hwang, Jae-Han Jeon, Sang Gyu Kwak, Donghwi Park, Jun Sung Moon
-
Endocrinol Metab. 2020;35(3):595-601. Published online August 26, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.719
-
-
7,029
View
-
182
Download
-
16
Web of Science
-
16
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Coronavirus disease 2019 (COVID-19) has become a global pandemic, which prompts a consensus for the necessity to seek risk factors for this critical disease. Risk factors affecting mortality of the disease remain elusive. Diabetes and hyperglycemia are known to negatively affect a host’s antiviral immunity. We evaluated the relationship between a history of diabetes, fasting plasma glucose (FPG) levels and mortality among severely ill patients with COVID-19.
Methods
This was a retrospective cohort study that assessed 106 adult inpatients (aged ≥18 years) from two tertiary hospitals in Daegu, South Korea. The participants were transferred to tertiary hospitals because their medical condition required immediate intensive care. The demographic and laboratory data were compared between COVID-19 patients who survived and those who did not.
Results
Compared with the survivor group, age, and the proportions of diabetes, chronic lung disease and FPG were significantly higher in the deceased group. In the Cox proportional hazards regression model for survival analysis, FPG level and age were identified as significant predictors of mortality (P<0.05). The threshold values for predicting high mortality were age >68 years and FPG of 168 mg/dL, respectively. Among those without diabetes, high FPG remained a significant predictor of mortality (P<0.04).
Conclusion
High FPG levels significantly predicted mortality in COVID-19, regardless of a known history of diabetes. These results suggest intensive monitoring should be provided to COVID-19 patients who have a high FPG level.
-
Citations
Citations to this article as recorded by  - Fasting Plasma Glucose Levels at the Time of Admission Predict 90-Day
Mortality in Patients with Viral Pneumonia. A Prospective Study
Jie Xu, Jianyu Zhao, Liyuan Wu, Xinxin Lu
Experimental and Clinical Endocrinology & Diabetes.2023; 131(05): 290. CrossRef - Influence of Fasting Plasma Glucose Level on Admission of COVID-19 Patients: A Retrospective Study
Yingying Zhao, Huichun Xing, Yong Xu
Journal of Diabetes Research.2022; 2022: 1. CrossRef - The Role of Diabetes and Hyperglycemia on COVID-19 Infection Course—A Narrative Review
Evangelia Tzeravini, Eleftherios Stratigakos, Chris Siafarikas, Anastasios Tentolouris, Nikolaos Tentolouris
Frontiers in Clinical Diabetes and Healthcare.2022;[Epub] CrossRef - Novel Glycemic Index Based on Continuous Glucose Monitoring to Predict Poor Clinical Outcomes in Critically Ill Patients: A Pilot Study
Eun Yeong Ha, Seung Min Chung, Il Rae Park, Yin Young Lee, Eun Young Choi, Jun Sung Moon
Frontiers in Endocrinology.2022;[Epub] CrossRef - Heterogeneity and Risk of Bias in Studies Examining Risk Factors for Severe Illness and Death in COVID-19: A Systematic Review and Meta-Analysis
Abraham Degarege, Zaeema Naveed, Josiane Kabayundo, David Brett-Major
Pathogens.2022; 11(5): 563. CrossRef - Global, Regional and National Burden of Cancers Attributable to High Fasting Plasma Glucose in 204 Countries and Territories, 1990-2019
Saeid Safiri, Seyed Aria Nejadghaderi, Nahid Karamzad, Jay S. Kaufman, Kristin Carson-Chahhoud, Nicola Luigi Bragazzi, Mark J. M. Sullman, Mohammad Reza Beyranvand, Mohammad Ali Mansournia, Amir Almasi-Hashiani, Gary S. Collins, Ali-Asghar Kolahi
Frontiers in Endocrinology.2022;[Epub] CrossRef - COVID-19 and diabetes—Two giants colliding: From pathophysiology to management
Maria Chiara Pelle, Isabella Zaffina, Michele Provenzano, Giovenale Moirano, Franco Arturi
Frontiers in Endocrinology.2022;[Epub] CrossRef - SARS-CoV-2 omicron variant clearance delayed in breakthrough cases with elevated fasting blood glucose
Xiujun Zhang, Guocan Si, Huifen Lu, Wei Zhang, Shuqin Zheng, Zeyu Huang, Longgen Liu, Yuan Xue, Guojun Zheng
Virology Journal.2022;[Epub] CrossRef - Hyperglycemia is Associated With Increased Mortality in Critically Ill Patients With COVID-19
Alon Y. Mazori, Ilana Ramer Bass, Lili Chan, Kusum S. Mathews, Deena R. Altman, Aparna Saha, Howard Soh, Huei Hsun Wen, Sonali Bose, Emily Leven, Jing Gennie Wang, Gohar Mosoyan, Pattharawin Pattharanitima, Giampaolo Greco, Emily J. Gallagher
Endocrine Practice.2021; 27(2): 95. CrossRef - The common risk factors for progression and mortality in COVID-19 patients: a meta-analysis
Li Zhang, Jie Hou, Fu-Zhe Ma, Jia Li, Shuai Xue, Zhong-Gao Xu
Archives of Virology.2021; 166(8): 2071. CrossRef - Dyslipidaemia and mortality in COVID-19 patients: a meta-analysis
M Zuin, G Rigatelli, C Bilato, C Cervellati, G Zuliani, L Roncon
QJM: An International Journal of Medicine.2021; 114(6): 390. CrossRef - National early warning score on admission as risk factor for invasive mechanical ventilation in COVID-19 patients
Min Cheol Chang, Tae Uk Kim, Donghwi Park
Medicine.2021; 100(19): e25917. CrossRef - Thyroid Hormone Profile and Its Prognostic Impact on the Coronavirus Disease 2019 in Korean Patients
Jiyeon Ahn, Min Kyung Lee, Jae Hyuk Lee, Seo Young Sohn
Endocrinology and Metabolism.2021; 36(4): 769. CrossRef - Diabetes, hypertension, body mass index, smoking and COVID-19-related mortality: a systematic review and meta-analysis of observational studies
Yahya Mahamat-Saleh, Thibault Fiolet, Mathieu Edouard Rebeaud, Matthieu Mulot, Anthony Guihur, Douae El Fatouhi, Nasser Laouali, Nathan Peiffer-Smadja, Dagfinn Aune, Gianluca Severi
BMJ Open.2021; 11(10): e052777. CrossRef - COVID-19 und Diabetes: Folgen der Pandemie
Baptist Gallwitz, Wolfgang Rathmann
Deutsches Ärzteblatt Online.2021;[Epub] CrossRef - Incidence of Post-Traumatic Stress Disorder after Coronavirus Disease
Min Cheol Chang, Donghwi Park
Healthcare.2020; 8(4): 373. CrossRef
- Clinical Study
- A Novel Index Using Soluble CD36 Is Associated with the Prevalence of Type 2 Diabetes Mellitus: Comparison Study with Triglyceride-Glucose Index
-
Ho Jin Kim, Jun Sung Moon, Il Rae Park, Joong Hee Kim, Ji Sung Yoon, Kyu Chang Won, Hyoung Woo Lee
-
Endocrinol Metab. 2017;32(3):375-382. Published online September 18, 2017
-
DOI: https://doi.org/10.3803/EnM.2017.32.3.375
-
-
4,716
View
-
47
Download
-
9
Web of Science
-
12
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Plasma soluble cluster determinant 36 (sCD36) level is closely related with insulin resistance and atherosclerosis, but little is known whether it could be a surrogate for estimating risk of developing diabetes or not. To address this, we evaluated association between sCD36 index, the product of sCD36 and fasting plasma glucose (FPG), and the prevalence of type 2 diabetes mellitus (T2DM), and then compared with triglyceride-glucose (TyG) index which has been suggested simple index for insulin resistance. MethodsThis was cross-sectional study, and participants were classified as normal glucose tolerance (NGT), prediabetes, and T2DM according to glucose tolerance. The formula of TyG index was ‘ln [FPG (mg/dL)×triglyceride (mg/dL)/2],’ and the sCD36 index was ‘ln [sCD36 (pg/mL)×FPG (mg/dL)/2].’ ResultsOne hundred and fifty-five subjects (mean age, 55.2 years) were enrolled, and patients with T2DM were 75. Both indexes were significantly increased in prediabetes and T2DM rather than NGT, and sCD36 index was positively correlated with both glycosylated hemoglobin and homeostasis model assessment of insulin resistance (r=0.767 and r=0.453, respectively; P<0.05) and negatively with homeostasis model assessment estimate of β-cell function (r=−0.317). The odds ratio (OR) of sCD36 index for T2DM was 4.39 (95% confidential interval, 1.51 to 12.77) after adjusting age, gender, blood pressure, smoking, alcohol, non-high density lipoprotein cholesterol and high-sensitivity C-reactive protein. However, OR of TyG index did not remained significance after adjustment. ConclusionsCD36 index has an independent association with the risk of T2DM, and showed better correlation than TyG index. These results suggest sCD36 index might be useful surrogate marker for the risk of diabetes.
-
Citations
Citations to this article as recorded by  - The triglyceride-glucose index as an indicator of insulin resistance and cardiometabolic risk in Brazilian adolescents
Miriam Beatrís Reckziegel, Patrik Nepomuceno, Tania Machado, Jane Dagmar Pollo Renner, Hildegard Hedwig Pohl, Carlos Alberto Nogueira-de-Almeida, Elza Daniel de Mello
Archives of Endocrinology and Metabolism.2023;[Epub] CrossRef - The association of soluble cluster of differentiation 36 with metabolic diseases: A potential biomarker and therapeutic target
Yun Li, Yaxi Chen, Xiong Z. Ruan
Pediatric Discovery.2023;[Epub] CrossRef - Kidney lipid dysmetabolism and lipid droplet accumulation in chronic kidney disease
Alla Mitrofanova, Sandra Merscher, Alessia Fornoni
Nature Reviews Nephrology.2023; 19(10): 629. CrossRef - Diabetic cardiac autonomic neuropathy: insulin resistance, lipid profile, and omega-3 polyunsaturated fatty acids
Martin-Yurii Markevich, Volodymyr Segin, Victoria Serhiyenko, Alexandr Serhiyenko
InterConf.2023; (35(163)): 213. CrossRef - Insulin resistance estimated by estimated glucose disposal rate predicts outcomes in acute ischemic stroke patients
Zhengzhao Lu, Yunyun Xiong, Xueyan Feng, Kaixuan Yang, Hongqiu Gu, Xingquan Zhao, Xia Meng, Yongjun Wang
Cardiovascular Diabetology.2023;[Epub] CrossRef - Usefulness of SPISE Index for Screening and Detection of Early Stages of Insulin Resistance among Chilean Young Adults
Isabel Pereyra González, Sandra Lopez-Arana
Annals of Nutrition and Metabolism.2023; 79(4): 372. CrossRef - Oxidative Stress Induced by Lipotoxicity and Renal Hypoxia in Diabetic Kidney Disease and Possible Therapeutic Interventions: Targeting the Lipid Metabolism and Hypoxia
Seung Yun Chae, Yaeni Kim, Cheol Whee Park
Antioxidants.2023; 12(12): 2083. CrossRef - Proteomic analysis of epicardial adipose tissue from heart disease patients with concomitant heart failure with preserved ejection fraction
Shan He, Huagang Zhu, Jianjun Zhang, Xiaopeng Wu, Lei Zhao, Xinchun Yang
International Journal of Cardiology.2022; 362: 118. CrossRef - DIABETIC CARDIAC AUTONOMIC NEUROPATHY: SIMVASTATIN, INSULIN RESISTANCE AND LIPIDS
Victoria Serhiyenko, Marta Hotsko, Samir Ajmi, Alexandr Serhiyenko
InterConf.2022; (18(95)): 531. CrossRef - New insights into renal lipid dysmetabolism in diabetic kidney disease
Alla Mitrofanova, George Burke, Sandra Merscher, Alessia Fornoni
World Journal of Diabetes.2021; 12(5): 524. CrossRef - The Role of CD36 in Type 2 Diabetes Mellitus: β-Cell Dysfunction and Beyond
Jun Sung Moon, Udayakumar Karunakaran, Elumalai Suma, Seung Min Chung, Kyu Chang Won
Diabetes & Metabolism Journal.2020; 44(2): 222. CrossRef - The Multifunctionality of CD36 in Diabetes Mellitus and Its Complications—Update in Pathogenesis, Treatment and Monitoring
Kamila Puchałowicz, Monika Ewa Rać
Cells.2020; 9(8): 1877. CrossRef
- Obesity and Metabolism
- Variation in Serum Creatinine Level Is Correlated to Risk of Type 2 Diabetes
-
Jun Sung Moon, Ji Eun Lee, Ji Sung Yoon
-
Endocrinol Metab. 2013;28(3):207-213. Published online September 13, 2013
-
DOI: https://doi.org/10.3803/EnM.2013.28.3.207
-
-
4,185
View
-
47
Download
-
19
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Skeletal muscle is well established as a major target organ of insulin action, and is associated with the pathogenesis of type 2 diabetes. Therefore, we attempted to determine whether a variation in serum creatinine is related to the development of type 2 diabetes and other risk factors for diabetes. MethodsA total of 2,676 nondiabetic subjects with stable and normal renal function (estimated glomerular filtration rate >60 mL/min/1.73 m2) were followed up for approximately 4.5 years. New onset diabetes was defined as fasting plasma glucose (FPG) ≥7.0 mmol/L, glycated hemoglobin (HbA1c) ≥6.5%, or subjects taking antidiabetic agents. Variation of serum creatinine (ΔCre) was defined as a difference between follow-up and baseline creatinine. In subgroup analysis, body composition was examined by bioelectric impedance analysis method. ResultsA total of 106 subjects were diagnosed with new-onset diabetes during the follow-up period. Baseline serum creatinine was not different between the new-onset diabetes and no diabetes groups. Negative ΔCre (ΔCre <0) showed an association with increased risk of type 2 diabetes after adjusting for age, sex, body mass index, systolic blood pressure, FPG, HbA1c, triglyceride, high density lipoprotein cholesterol, and γ-glutamyl transpeptidase (odds ratio, 1.885; 95% confidence interval, 1.127 to 3.153). Serum creatinine level demonstrated positive correlation with muscle mass and negative correlation with percentage of body fat in body composition analysis. ConclusionSerum creatinine reflected body muscle mass and the decrease of serum creatinine might be regarded as a risk factor for type 2 diabetes.
-
Citations
Citations to this article as recorded by  - Low serum creatinine, a surrogate marker of muscle mass, correlates with insulin sensitivity in nonhuman primates
Uddhav K. Chaudhari, Barbara C. Hansen
Journal of Medical Primatology.2023; 52(2): 100. CrossRef - Identification of Novel Biomarkers of Spinal Muscular Atrophy and Therapeutic Response by Proteomic and Metabolomic Profiling of Human Biological Fluid Samples
Megi Meneri, Elena Abati, Delia Gagliardi, Irene Faravelli, Valeria Parente, Antonia Ratti, Federico Verde, Nicola Ticozzi, Giacomo P. Comi, Linda Ottoboni, Stefania Corti
Biomedicines.2023; 11(5): 1254. CrossRef - Association of serum creatinine levels and risk of type 2 diabetes mellitus in Korea: a case control study
Do Kyeong Song, Young Sun Hong, Yeon-Ah Sung, Hyejin Lee
BMC Endocrine Disorders.2022;[Epub] CrossRef - Impact of Female Sex on the Susceptibility to Hypernatremia Among Older Community-Dwelling Individuals in Japan
Sho Tanaka, Midori Fujishiro, Kazuhiro Imatake, Yasuyuki Suzuki, Hisamitsu Ishihara, Shigemasa Tani
International Journal of General Medicine.2022; Volume 15: 777. CrossRef - Ameliorative Effect of Oxytocin on FBN1 and PEPCK Gene Expression, and Behavioral Patterns in Rats' Obesity-Induced Diabetes
Asmaa Elnagar, Khalifa El-Dawy, Hussein I. El-Belbasi, Ibrahim F. Rehan, Hamdy Embark, Zeinab Al-Amgad, Obeid Shanab, Elsayed Mickdam, Gaber E. Batiha, Salman Alamery, Samer S. Fouad, Simona Cavalu, Mohammed Youssef
Frontiers in Public Health.2022;[Epub] CrossRef - Time to doubling of serum creatinine in patients with diabetes in Ethiopian University Hospital: Retrospective follow-up study
Adeladlew Kassie Netere, Ashenafi Kibret Sendekie, Donovan Anthony McGrowder
PLOS ONE.2022; 17(9): e0274495. CrossRef - Deep Learning for Integrated Analysis of Insulin Resistance with Multi-Omics Data
Eunchong Huang, Sarah Kim, TaeJin Ahn
Journal of Personalized Medicine.2021; 11(2): 128. CrossRef - Arsenic Secondary Methylation Capacity Is Inversely Associated with Arsenic Exposure-Related Muscle Mass Reduction
Md. Khalequzzaman Sarker, Selim Reza Tony, Abu Eabrahim Siddique, Md. Rezaul Karim, Nazmul Haque, Zohurul Islam, Md. Shofikul Islam, Moriom Khatun, Jahidul Islam, Shakhawoat Hossain, Zahangir Alam Saud, Hideki Miyataka, Daigo Sumi, Aaron Barchowsky, Seiic
International Journal of Environmental Research and Public Health.2021; 18(18): 9730. CrossRef - Creatinine to Body Weight Ratio Is Associated with Incident Diabetes: Population-Based Cohort Study
Yoshitaka Hashimoto, Takuro Okamura, Masahide Hamaguchi, Akihiro Obora, Takao Kojima, Michiaki Fukui
Journal of Clinical Medicine.2020; 9(1): 227. CrossRef - ¿Debemos prestar más atención a la creatinina baja?
Carlos A. Amado Diago, José A. Amado Señaris
Endocrinología, Diabetes y Nutrición.2020; 67(7): 486. CrossRef - Arsenic exposure-related hyperglycemia is linked to insulin resistance with concomitant reduction of skeletal muscle mass
Victor Mondal, Zubaer Hosen, Faruk Hossen, Abu Eabrahim Siddique, Selim Reza Tony, Zohurul Islam, Md. Shofikul Islam, Shakhawoat Hossain, Khairul Islam, Md. Khalequzzaman Sarker, M.M. Hasibuzzaman, Ling-Zhi Liu, Bing-Hua Jiang, Md Mominul Hoque, Zahangir
Environment International.2020; 143: 105890. CrossRef - Noninvasive assessment of abdominal adipose tissues and quantification of hepatic and pancreatic fat fractions in type 2 diabetes mellitus
Manoj Kumar Sarma, Andres Saucedo, Christine Hema Darwin, Ely Richard Felker, Kavya Umachandran, Daniel Kohanghadosh, Edward Xu, Steve Raman, Michael Albert Thomas
Magnetic Resonance Imaging.2020; 72: 95. CrossRef - Should we pay more attention to low creatinine levels?
Carlos A. Amado Diago, José A. Amado Señaris
Endocrinología, Diabetes y Nutrición (English ed.).2020; 67(7): 486. CrossRef - Acute Effect of the Timing of Resistance Exercise and Nutrient Intake on Muscle Protein Breakdown
Wataru Kume, Jun Yasuda, Takeshi Hashimoto
Nutrients.2020; 12(4): 1177. CrossRef - Serum creatinine levels and risk of incident type 2 diabetes mellitus or dysglycemia in middle-aged Japanese men: a retrospective cohort study
Mamoru Takeuchi, Hironori Imano, Isao Muraki, Yuji Shimizu, Mina Hayama-Terada, Akihiko Kitamura, Takeo Okada, Masahiko Kiyama, Hiroyasu Iso
BMJ Open Diabetes Research & Care.2018; 6(1): e000492. CrossRef - Assessment of kidney dysfunction with cystatin C- and creatinine-based estimated glomerular filtration rate and predicting type 2 diabetes: Toranomon Hospital Health Management Center Study 21
Yoriko Heianza, Shigeko Hara, Kazumi Saito, Hiroshi Tsuji, Shiro Tanaka, Satoru Kodama, Tetsuro Kobayashi, Yasuji Arase, Hirohito Sone
Diabetes Research and Clinical Practice.2016; 113: 60. CrossRef - Profiling human blood serum metabolites by nuclear magnetic resonance spectroscopy: a comprehensive tool for the evaluation of hemodialysis efficiency
Marika Kromke, Martina Palomino-Schätzlein, Horst Mayer, Stefan Pfeffer, Antonio Pineda-Lucena, Burkhard Luy, Martin Hausberg, Claudia Muhle-Goll
Translational Research.2016; 171: 71. CrossRef - Safety evaluation of the consumption of high dose milk fat globule membrane in healthy adults: a double-blind, randomized controlled trial with parallel group design
Sayaka Hari, Ryuji Ochiai, Yasushi Shioya, Yoshihisa Katsuragi
Bioscience, Biotechnology, and Biochemistry.2015; 79(7): 1172. CrossRef - Brief Review of Articles in 'Endocrinology and Metabolism' in 2013
Won-Young Lee
Endocrinology and Metabolism.2014; 29(3): 251. CrossRef
|